
Only after you do ultrasound you can do a vaginal exam to feel for cervical dilation, presence of fetal head at cervical opening (crowning), and presence of cord prolapse. If present, the patient cannot proceed with vaginal delivery and needs a c-section. Placental previa can be rapidly identified using ultrasound. Look for vertex positioning of the fetus (headfirst) and look for position of the placenta. 
6g loading dose over 20 minutes, followed by 1-2g per hour based on serum creatinine.īedside ultrasound should be rapidly performed prior to any vaginal examination, in addition to patient history, so as to avoid examining a placenta previa or low-lying placenta which may result in vaginal bleeding. If elevated BP plus one of these is present, the patient requires prompt magnesium drip even as delivery is occurring. Ask the patient if she has hand or facial edema. Further check for degree of proteinuria, headache, blurry vision, chest or epigastric or RUQ pain are suggestive of preeclampsia. If SBP >140 or DBP >90, have a high suspicion for preeclampsia in the patient who does not have previously diagnosed chronic hypertension. Any fever on assessment could be an intra-amniotic infection and obviously requires immediate antibiotic therapy.ĭetermine rupture of membranes: if convinced the patient has ruptured the amniotic membrane, and if this occurred >18 hours, start antibiotic coverage ASAP. GBS Prophylaxis: If you think the patient is 37 weeks, or you have their due date in the EMR, then antibiotics are unnecessary. Ask about penicillin allergies (relevant for GBS prophylaxis). Medical/Obstetric problems: ask about previous c-sections (prior classical incisions on the skin carry an ~8% future risk of rupture), any present pregnancy fetal anomalies, maternal bleeding issues, preeclampsia, gestational or chronic hypertension, placental abruption. For the record, ectopic pregnancies do not count. “ Florida Power And Light ( Full term, Pre-term, Abortions, Living)”. Any fetus born 20w0d, summarized below): remember this cool mnemonic for asking about G’s and P’s. GA is critical because it prepares you for how to anticipate the type of delivery and the neonatal care needed. Simplifying this more, if palpable above the umbilicus, then the pregnancy is likely >20 weeks. This method works best in those with a body habitus that allows this form of measuring. For example, if you measure using your fingertip 24 cm above the pubic symphysis at the uterine fundus, the pregnancy is ~24 weeks in gestational age. Let’s say you are unable to talk to the patient due to their clinical condition or language barrier palpate the abdomen for the uterine fundus. These are all over the internet and ( ACOG Calculator). Gestational age: if only the estimated due date or the last menstrual cycle is available, you can use a calculator to find the current age. Rapid OB/GYN history: you can do this fast and it helps you understand any prior issues the mother may have had. Don’t forget to call pediatrics (neonatology is preferred if available). Calling for help is quite obvious to anyone who is not an obstetrician. Hitherto, you are stuck managing this situation. Head flexion and descent internal rotation extension external rotation delivery of anterior shoulder delivery of posterior shoulderįirst step: Call for help. “Call for transfer” is more likely to be the first option considered by many EM physicians, but this review assumes the mother is active labor (see below for details what that means). 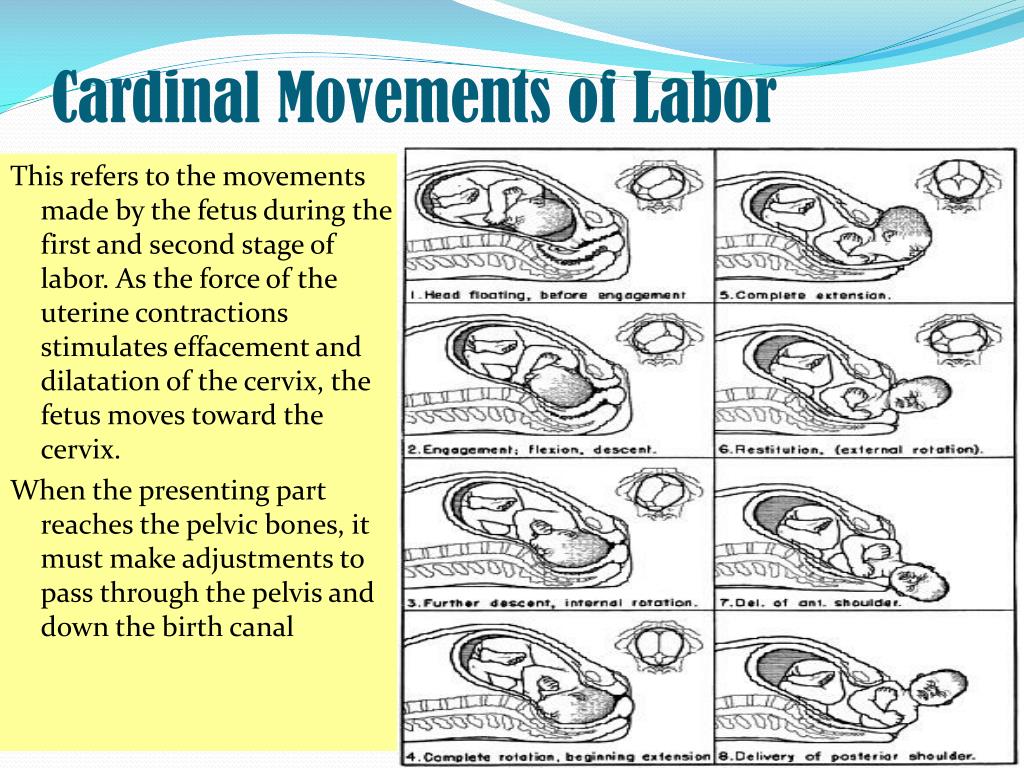
Precipitous delivery = labor no more than 3 hours from the onset of regular contractions.Ĭardinal movements of the fetus during the birth process are commonly tested on EM boards. If you are working in any ED, there is a high chance in your career at some point you will manage an unexpected labor & delivery, often with no OB/GYN available. You can read more about him at the end of the review. Briggs (senior) is an MFM specialist with >25 years of community experience. We wanted to make sure we covered the most up-to-date information, so we asked a friend to join us. This review serves as a guide to the emergency physician in managing precipitous labor. Infants died in droves, and maternal morbidity & mortality was substantial. It is interesting to think for tens of thousands of years we delivered babies outside the hospital setting prior to the advent of modern medicine, but this was not without cost. 
In the majority of cases, all goes well and thankfully mother and baby have good outcomes. Want to experience the greatest in board studying? Check out our interactive question bank podcast- the FIRST of its kind here: Įven in the US, hundreds of deliveries per year occur precipitously in emergency departments and even outside the hospital setting.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
